Ozempic vs Metformin: Comparison for Diabetes Treatment
Managing diabetes effectively often requires the use of medications to help control blood sugar levels. Two popular options for treating type 2 diabetes are Ozempic and metformin. These drugs have been proven effective in lowering blood glucose, but they differ in several ways, making it essential for individuals and healthcare providers to understand their benefits […]
Managing diabetes effectively often requires the use of medications to help control blood sugar levels. Two popular options for treating type 2 diabetes are Ozempic and metformin. These drugs have been proven effective in lowering blood glucose, but they differ in several ways, making it essential for individuals and healthcare providers to understand their benefits and risks when deciding on a suitable treatment plan.
Ozempic, known generically as semaglutide, is a hormone injection that works by mimicking the effects of a hormone called GLP-1 to stimulate insulin production, while metformin is an oral medication that primarily helps the body use insulin more efficiently. Although both medications strive to achieve blood sugar control, their mechanisms of action, side effects, and additional benefits like weight management may vary, which can impact their suitability for different patients and situations.
Comparing Ozempic and metformin can provide valuable insights into their distinct features and potential usage for people with type 2 diabetes. By understanding how each medication works and considering factors such as efficacy, side effects, and cost, patients and healthcare providers can make informed decisions on the most appropriate treatment option to manage diabetes effectively and maintain a high quality of life.
What Is Ozempic and What Is Metformin
Ozempic and Metformin are both FDA-approved medications used to manage type 2 diabetes. They help control blood sugar levels, and their mechanisms of action are different, thus catering to unique patient needs.
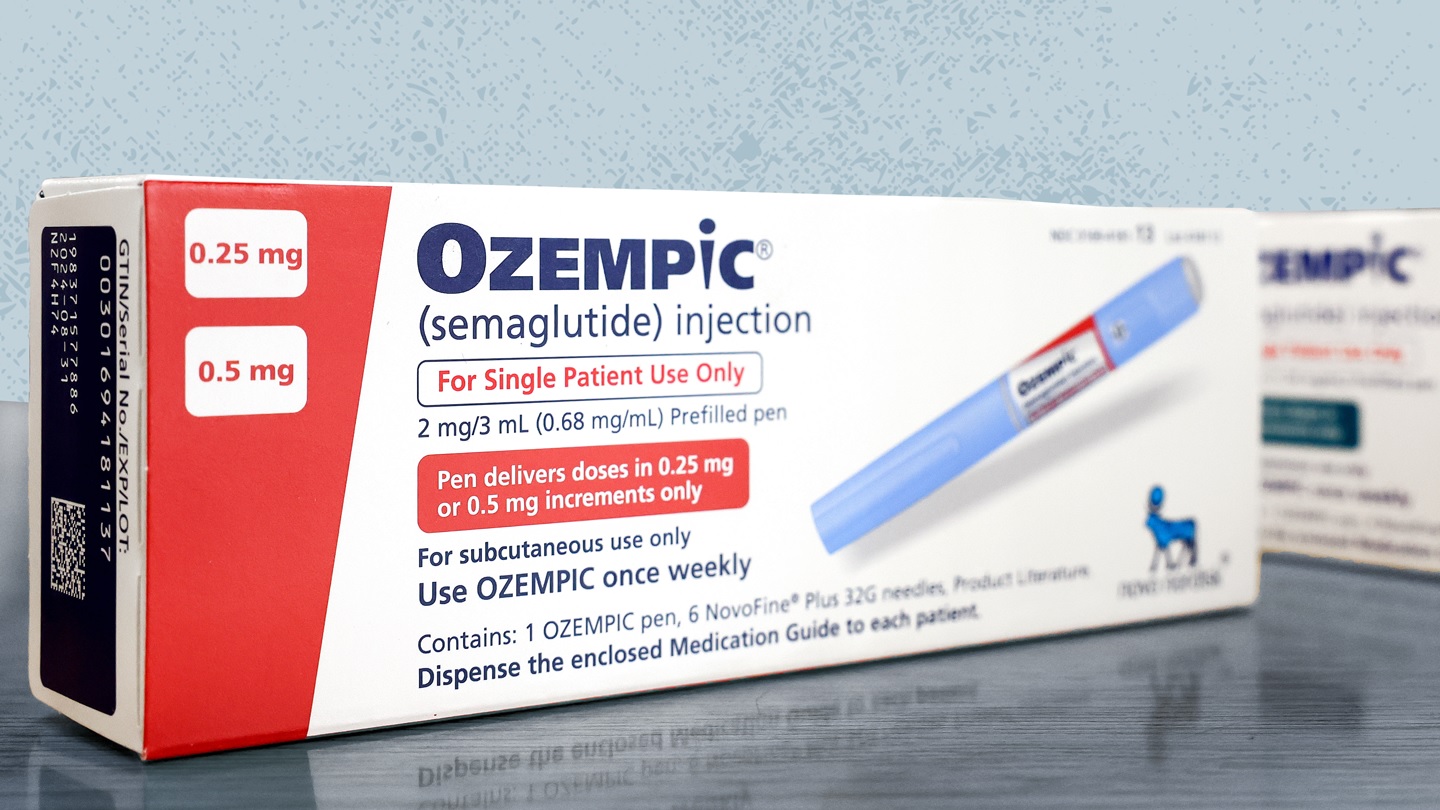
Ozempic (semaglutide) is a glucagon-like peptide-1 (GLP-1) receptor agonist. It works by mimicking the action of the natural hormone GLP-1, which increases insulin secretion and reduces the production of glucose in the liver. As a result, blood sugar levels are better regulated. Besides managing type 2 diabetes, Ozempic has been shown to promote weight loss and reduce cardiovascular risks in those with heart disease. Other GLP-1 receptor agonists include Trulicity, Victoza, Bydureon BCise, and Wegovy. Recently, the FDA has also approved a pill version of semaglutide called Rybelsus.
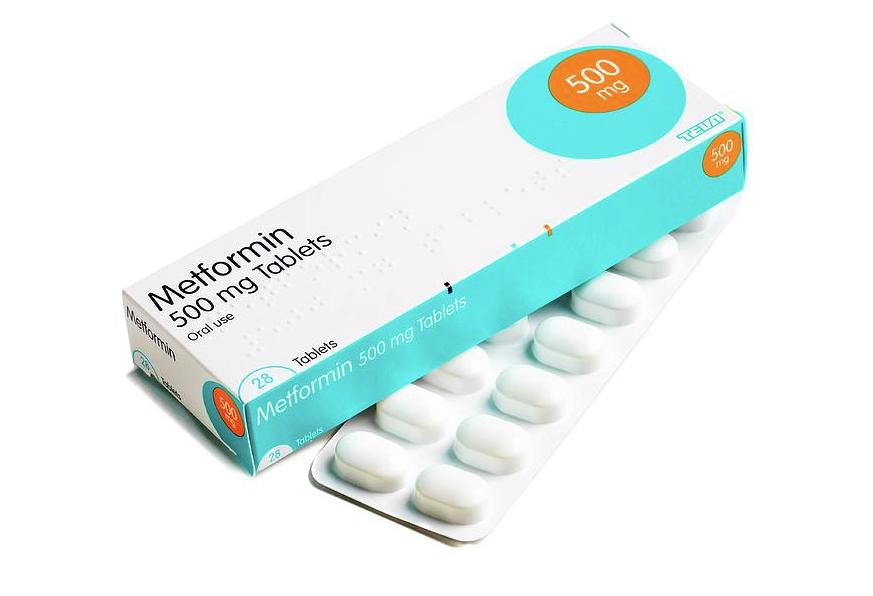
Metformin is a widely used, first-line medication for type 2 diabetes. It primarily works by decreasing the amount of glucose produced by the liver and increasing the sensitivity of muscle cells to insulin. This allows better utilization of glucose by the cells, thus keeping blood sugar levels in check. The popularity of metformin is partly due to its affordability and established efficacy over decades.
While both Ozempic and Metformin are effective in managing diabetes, they can be used in combination or as standalone treatments, depending on individual needs. Metformin is often employed as an initial treatment, while Ozempic may be considered for patients who require additional blood sugar control or have cardiovascular risks. It is essential to work closely with a healthcare professional to determine the best course of action based on one’s unique medical history and preferences.
How Ozempic and Metformin Work
Ozempic and metformin are both medications used to manage and control blood sugar levels in people with type 2 diabetes. Although they serve a similar purpose, they work in distinct ways to achieve these similar goals.
Ozempic, also known as semaglutide, is a medication that belongs to the glucagon-like peptide-1 (GLP-1) receptor agonist class of drugs. It works by mimicking the action of a naturally occurring hormone called GLP-1. This hormone is involved in the regulation of blood glucose, as it stimulates the release of insulin while suppressing the release of glucagon, a hormone that increases blood sugar levels. By doing so, Ozempic helps lower blood sugar levels in patients with type 2 diabetes.
Metformin, on the other hand, falls under the class of drugs known as biguanides. It functions differently from Ozempic, primarily acting on the liver. Metformin reduces glucose production in the liver and also increases insulin sensitivity in the muscles, promoting the uptake of glucose from the bloodstream. This, in turn, contributes to lower blood glucose levels in individuals with type 2 diabetes.
Both Ozempic and metformin also have an impact on the kidneys. Ozempic increases the volume of glucose excreted through urine by affecting the reabsorption of glucose in the kidney’s tubules. In contrast, metformin’s impact on the kidneys is minimal, as its primary site of action is the liver.
In summary, Ozempic and metformin are effective medications in managing type 2 diabetes and lowering blood glucose levels. They work through different mechanisms, with Ozempic acting as a GLP-1 receptor agonist and metformin as a biguanide. Both medications influence various organs, such as the liver and kidneys, to achieve their desired effects in regulating blood sugar levels.
Side Effects of Ozempic and Metformin
Ozempic and metformin are both medications used to treat type 2 diabetes, but they can cause different side effects for some patients. Common side effects of metformin include abdominal pain, nausea, vomiting, and diarrhea. Additionally, it may cause bloating, headache, weakness, and low blood sugar (hypoglycemia). In rare cases, metformin has a risk of lactic acidosis, a serious and potentially life-threatening condition.
On the other hand, Ozempic is known to cause nausea, vomiting, and diarrhea, similar to metformin. However, it can also lead to constipation and abdominal pain. In rare cases, Ozempic has been linked to pancreatitis, gallbladder disease, and an increased risk of developing thyroid c-cell tumors. It’s important to note that these serious side effects are not common and occur infrequently.
Both medications may affect blood sugar levels, but on different levels. Metformin can lower blood sugar, while Ozempic helps regulate it4. It’s worth mentioning that diabetes patients might experience complications like heart disease, heart attack, stroke, kidney disease, and diabetic retinopathy. However, these complications are results of the disease itself and not direct side effects of the medications.
In summary, metformin and Ozempic share some common side effects like nausea, vomiting, and diarrhea. Metformin might cause additional side effects like bloating, headache, weakness, and hypoglycemia. In rare cases, it can cause lactic acidosis. Ozempic, on the other hand, may result in constipation and abdominal pain. Serious but rare side effects of Ozempic include pancreatitis, gallbladder disease, and thyroid c-cell tumors. Monitoring and management of side effects is crucial for those using these medications to treat type 2 diabetes.
Administration and Dosage
Ozempic and metformin are both medications used for the treatment of Type 2 diabetes, but they differ in their administration and dosages.
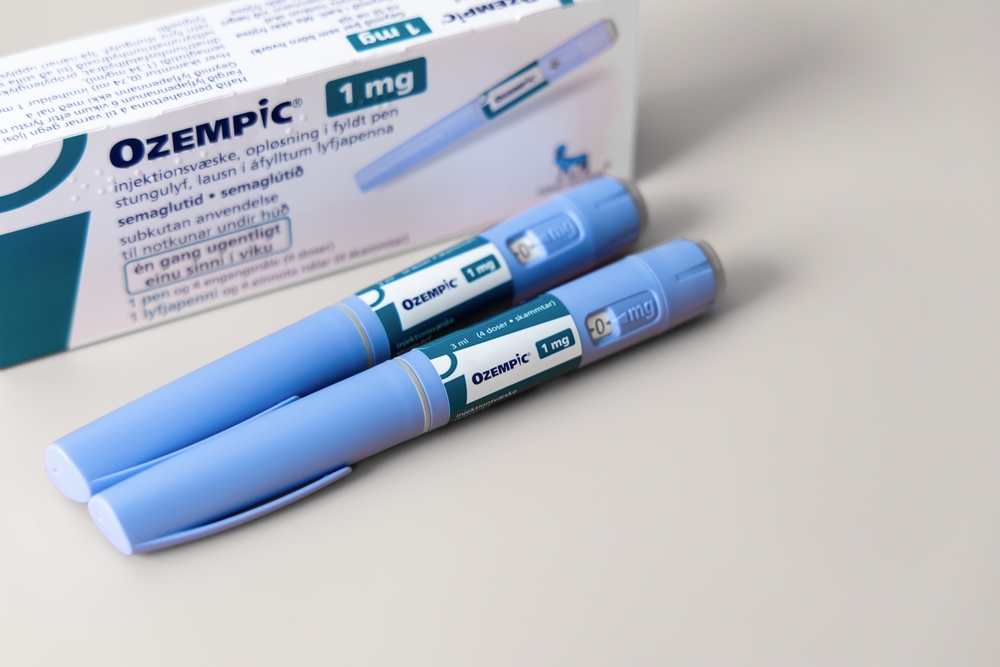
Ozempic (semaglutide) is a once-weekly injection. It is administered as a subcutaneous injection, usually in the thigh, upper arm, or abdomen. The initial dosage for Ozempic is 0.25 mg per week for the first four weeks, and then it is increased to 0.5 mg per week. Depending on the patient’s individual needs and A1C levels, the dosage may be further increased to 1 mg per week under medical supervision.
Metformin, on the other hand, is an oral medication available in various forms, including immediate-release and extended-release tablets as well as a liquid oral suspension. The immediate-release tablet is typically taken twice a day with meals, while the extended-release tablet is usually taken once a day with an evening meal. The starting dosage for metformin is often 500 mg per day, which can be gradually increased up to 2000-2500 mg daily, depending on the patient’s tolerance and A1C levels.
When it comes to determining the most effective dosages for both Ozempic and metformin, it is essential to monitor blood glucose levels regularly and adjust the dosages accordingly. This process must be done under the guidance of a healthcare professional to ensure optimal results and avoid potential complications. Overall, while the administration and dosage of these two medications differ, their ultimate goal is to lower blood glucose levels and assist in managing Type 2 diabetes.
Impact on Weight Management
Ozempic and Metformin are two medications that have garnered significant attention for their potential impact on weight management, especially in individuals with obesity or those who are overweight. Both drugs were initially developed to treat diabetes, but have also been found to be helpful in managing weight.
Ozempic, also known as semaglutide, is a relatively newer hormonal treatment that has shown promising results in helping patients lose weight. It works by changing the way a person’s body reacts to food, subsequently making it easier for them to feel full and reduce their overall food intake. In a study examining the effects of Ozempic on weight loss, participants lost an average of 17.4% of their original weight in 14 months.
On the other hand, Metformin is a more affordable and widely-used diabetes medication that has also been found to aid in weight loss. Its primary function is regulating blood sugar levels, which can in turn help patients manage their weight. In a study on Metformin’s effects on weight management, participants experienced a 5.6% weight reduction in just 6 months. However, it should be noted that these drugs were not compared directly, and the duration of the studies varied.
Besides the difference in weight loss percentages, Ozempic and Metformin have distinct mechanisms of action and potential benefits. For instance, Ozempic can lower the risk of heart attack and stroke in patients with diabetes and heart disease, while also offering possible kidney benefits. Metformin, being a first-choice medication for type 2 diabetes, primarily focuses on the regulation of blood sugar levels.
In summary, both Ozempic and Metformin have demonstrated efficacy in weight management for patients struggling with obesity or being overweight. Despite their differences in mechanisms, both medications may provide a useful means of maintaining a healthier body weight in conjunction with a balanced diet and regular exercise.
Interactions with Other Drugs
Ozempic and metformin are both medications used to treat type 2 diabetes. They work in different ways to help control blood sugar levels, and can be prescribed separately or together. However, it is essential to be aware of potential drug interactions when taking these medications with other drugs.
Ozempic, also known as semaglutide, has specific contraindications to be aware of. For instance, it is not advised for those who have a personal or family history of thyroid cancer. Although Ozempic may cause nausea, vomiting, and diarrhea in some cases, it has also been linked to rare instances of pancreatitis and gallbladder disease.
Metformin, on the other hand, is a more commonly prescribed first-choice medication for type 2 diabetes and works by reducing the amount of sugar the liver releases into the bloodstream. While metformin has its own set of side effects, such as taste disturbances and gastrointestinal issues, there are certain medications that may interact with metformin and should be avoided:
- Antipsychotics: These medications, often used to treat mental health conditions, may increase blood sugar levels, thus affecting the efficacy of metformin.
- Carbonic Anhydrase Inhibitors: These drugs, used to treat glaucoma and other conditions, may increase the risk of lactic acidosis, a rare but serious side effect of metformin.
Patients taking sulfonylureas, a class of medications for type 2 diabetes that stimulate the pancreas to produce more insulin, should be cautious when combining them with metformin. This is because using both medications together may cause low blood sugar (hypoglycemia) due to their additive effects. To manage this risk, your doctor may adjust the dose of sulfonylurea or recommend monitoring blood sugar levels closely.
In summary, being aware of potential drug interactions is crucial for the safe and effective use of Ozempic and metformin. Consulting with a healthcare professional about current medications and any potential interactions will ensure the best possible diabetes management.
Usage in Special Populations
When it comes to the usage of Ozempic and metformin in special populations, there are a few factors to consider, such as age, pregnancy, breastfeeding, and the presence of other medical conditions.
Age and Children: Ozempic is approved for use in adults, while metformin is approved for both adults and children ages 10 and older. However, it is essential to consult with a healthcare professional before administering these medications to children, as the effectiveness and safety might vary depending on the child’s age and overall health condition.
Pregnancy and Breastfeeding: The safety of using Ozempic during pregnancy has not been extensively studied, and it is classified as a pregnancy category C drug, meaning that it may cause harm to the unborn baby. On the other hand, metformin is considered safe for use during pregnancy, as it is a pregnancy category B drug, suggesting that there is no evidence of harm to the fetus in animal studies. However, it is still crucial to discuss the risks and benefits of using these medications during pregnancy with a healthcare professional. Both Ozempic and metformin are not recommended during breastfeeding, as it is unknown whether they pass into breast milk and may pose a risk to the nursing infant.
High Blood Pressure: There is no direct contraindication for the use of Ozempic or metformin in patients with high blood pressure. However, it is essential to monitor blood pressure regularly while taking these medications, as improved blood sugar control may lead to a reduction in blood pressure. Additionally, patients with high blood pressure should continue to follow their healthcare professional’s advice on managing their condition, which may include lifestyle modifications and other medications.
High Cholesterol: Both Ozempic and metformin have been shown to have beneficial effects on cholesterol levels. Ozempic has been reported to reduce LDL cholesterol (bad cholesterol) and increase HDL cholesterol (good cholesterol), while metformin has been demonstrated to lower LDL cholesterol and total cholesterol levels. Nevertheless, it is crucial for patients with high cholesterol to continue adhering to their healthcare professional’s recommendations, which may include diet modifications, exercise, and the use of other cholesterol-lowering medications.
In conclusion, it is essential to consult with a healthcare professional before starting or changing medications, especially in special populations such as children, pregnant or breastfeeding women, and patients with high blood pressure or high cholesterol. A healthcare provider will be able to recommend the most appropriate treatment option based on an individual’s specific needs and medical history.
Cost and Insurance Coverage
Ozempic and metformin are both medications used to treat Type 2 diabetes, but they differ significantly in cost and insurance coverage. Metformin is a more affordable option, whereas Ozempic is on the pricier side.
The retail price for Ozempic ranges from $1,000 to $1,200 or more for one pen, depending on the pharmacy. Insurance plans may cover Ozempic for treating Type 2 diabetes, but coverage may not be available for weight loss purposes. The cost for Ozempic typically runs between $0 and $995 per month, depending on the insurance plan, formulary, and deductibles or copays. Patients can also contact Novocare, a support program offered by Novo Nordisk, to receive Ozempic cost estimates.
On the other hand, metformin is a generic medication, making it more affordable for patients to obtain. Unlike Ozempic, metformin does not require any special forms of administration like injections, contributing to its cost-effectiveness.
Medicare and most insurance plans typically cover metformin, as it is a well-established and low-cost treatment for Type 2 diabetes. Patients may further reduce their out-of-pocket expenses for metformin by using available coupons from various sources.
In summary, while Ozempic and metformin both treat Type 2 diabetes, differences in cost and insurance coverage should be considered when choosing between these medications. Metformin represents a more budget-friendly option, whereas Ozempic may have a higher out-of-pocket expense for patients, depending on their insurance plans and unique needs.
Warnings and Precautions
When considering the use of Ozempic (semaglutide) and metformin for the treatment of type 2 diabetes, it’s essential to be aware of warnings and precautions associated with each medication.
Ozempic carries a warning for individuals with a personal or family history of medullary thyroid carcinoma (MTC) or multiple endocrine neoplasia syndrome type 2 (MEN 2). Patients with these conditions should not use Ozempic, as there could be an increased risk of developing MTC. Additionally, Ozempic should not be used in those with a known hypersensitivity to semaglutide or any other components of the medication.
Metformin, on the other hand, has a few different precautions. It is not recommended for individuals with severe kidney impairment or a history of metabolic acidosis, as these factors could increase the risk of lactic acidosis. Those with known hypersensitivity to metformin or its components should avoid its use as well.
Both medications have unique considerations related to interactions with other substances. Metformin should be used with caution during periods of fasting, as this could lead to an increased risk of low blood sugar (hypoglycemia). Additionally, alcohol consumption should be carefully monitored while taking metformin, as it may potentiate the medication’s effect on lactate metabolism, increasing the risk of lactic acidosis.
When using Ozempic, patients must be aware that this medication is a once-weekly injection, whereas metformin is an oral pill. This difference in administration may be a consideration for some individuals.
In conclusion, while Ozempic and metformin are both effective treatments for type 2 diabetes, it is crucial to consider the warnings and precautions associated with each medication. Understanding these factors can help in making an informed decision about the most suitable treatment option for each individual.
Diabetes Management and Lifestyle Factors
Diabetes management is crucial for individuals diagnosed with type 2 diabetes. Two prominent medications used for this purpose are Ozempic and Metformin. Both help in reducing blood sugar levels and improving insulin sensitivity, but they work in different ways and may have unique benefits.
Ozempic, a once-daily injectable medication, is known for its weight loss effects and its ability to lower the risk of heart attack and stroke among patients with diabetes and heart disease. It works by mimicking the hormone GLP-1, helping the body regulate hunger and ultimately controlling blood sugar levels.
Metformin, on the other hand, is a more common first-choice medication for type 2 diabetes and is often taken orally. Unlike Ozempic, it doesn’t directly affect appetite or weight loss. However, it functions by improving insulin sensitivity and reducing the amount of sugar produced by the liver.
In addition to medication, lifestyle adjustments play a significant role in diabetes management. Incorporating regular exercise and maintaining a balanced diet are essential for achieving optimal blood sugar control. Focusing on foods low in sugar and rich in fiber, along with portion control, can contribute to better glycemic control.
Physical activity allows the body to use insulin more effectively and helps in lowering blood sugar levels. Ideally, individuals with type 2 diabetes should engage in at least 150 minutes of moderate-intensity aerobic exercise per week, such as walking, swimming, or bicycling. Resistance training can also aid in building muscle mass, which improves insulin sensitivity.
Monitoring blood sugar levels is another essential aspect of diabetes management. Regular checks enable patients to understand how their body responds to specific foods, exercises, and medications. Additionally, monitoring the A1C levels – a metric that measures average blood glucose levels over the past two to three months – assists in tracking overall progress and identifying any necessary treatment adjustments.
In conclusion, both Ozempic and Metformin offer different advantages in diabetes management, and a combination of medication and lifestyle adjustments can help achieve better control of blood sugar levels. Regular exercise, a balanced diet, and close monitoring of blood sugar and A1C levels are key factors in mitigating the impact of type 2 diabetes.

Research and Studies
Recent studies have compared the efficacy and safety of Ozempic (semaglutide) and metformin in treating patients with type 2 diabetes. In a double-blind, phase 3a, randomized trial, researchers explored the benefits of once-weekly semaglutide versus once-daily sitagliptin as an add-on to metformin. This trial revealed semaglutide to be a potentially more effective option for some patients.
Another study showed that weight loss is more likely with Ozempic than with metformin. Furthermore, Ozempic has been found to lower the risk of heart attack and stroke in patients with diabetes and heart disease. It also demonstrates potential benefits for kidney health.
As for cancer, research concerning these two medications is limited. However, metformin has been associated with a reduced risk of certain types of cancer, while more research is needed to determine Ozempic’s effect on cancer risk. In terms of diabetic ketoacidosis, both drugs are designed to manage blood sugar levels and reduce the risk of this dangerous condition.
Regarding cardiovascular events, Ozempic stands out as it has shown to significantly reduce the risk of such events in patients with diabetes and heart disease. A review by the Canadian Agency for Drugs and Technologies in Health examined semaglutide’s efficacy in combination with metformin and sulfonylurea as a third-line treatment. It found this combination to be a promising option for improving glycemic control in adult patients with type 2 diabetes.
In summary, research indicates that both Ozempic and metformin have their own merits in treating type 2 diabetes. While metformin is a widely used first-choice medication, Ozempic has shown promising results in various areas, such as weight loss, kidney health, and cardiovascular event risk reduction. Both medications aim to manage blood sugar levels effectively to minimize the risk of diabetic ketoacidosis. Further research is required to fully understand their impact on cancer risk.
Patient Experience and Reviews
When it comes to patient experiences with Ozempic and Metformin, there are several factors to consider.
Efficacy: Both medications are effective in managing blood sugar levels, but their mechanisms of action are different. Ozempic, a newer medication, is an injectable glucagon-like peptide-1 (GLP-1) receptor agonist and has been shown to help with weight loss and lower the risk of heart attack and stroke in patients with diabetes and heart disease. Metformin, on the other hand, is an oral medication that has been a first-choice treatment for Type 2 diabetes for decades and has shown modest weight loss effects in some patients.
Side effects: Patients using Ozempic and Metformin may experience different side effects. For example, the most common side effects of Ozempic include nausea, vomiting, diarrhea, constipation, and abdominal pain. Metformin’s side effects are generally milder and can include gastrointestinal issues such as stomach pain, nausea, and diarrhea. However, these side effects usually decrease over time as the body adjusts to the medication.
Administration: Ozempic is an injectable medication, which may not be suitable for all patients, especially those who dislike needles or prefer oral medications. Metformin, in contrast, is taken as a pill, making it a more convenient option for many patients.
Cost and availability: While Metformin is widely available and generally affordable, Ozempic can be more difficult to obtain, even with a prescription. However, insurance coverage for both medications can vary, and it’s essential for the patients to discuss the prices and accessibility with their healthcare providers.
Personal preferences: As with any medication, individual experiences may vary. Some patients might find success with Ozempic, while others may prefer Metformin, or vice versa. It is essential for patients to communicate with their healthcare providers about their specific needs, preferences, and experiences with both medications to determine which one is the best fit.
In summary, both Ozempic and Metformin have their own unique properties that can benefit patients with type 2 diabetes. It’s essential to consider factors like efficacy, side effects, administration, cost, availability, and personal preferences when deciding which medication is the most suitable choice.
Vicky
I am a mother, wife, daughter, granddaughter, writer, living in Virginia Beach. I love creativity, ideas, crafts, arts, photography, movies, food, coffee, naps, outdoors. I love to make stuff!



